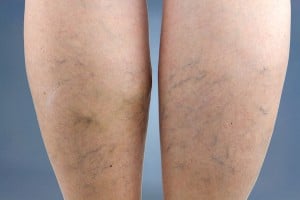
They are caused by swollen venules, arterioles, or capillaries and will somewhat differ in appearance depending on their location on the capillary loop. Telangiectasia along the arterioles will often appear small and bright red in appearance. They typically will not protrude above the surface. Those situated along the venules, however, are often blue and wider and may protrude above the skin.
Common causes
There are many types of telangiectasia and it can develop on any area of the body but it most commonly occurs around the nose, chin, and cheeks and the upper thigh, knee joint, and ankle areas. There are several things that can cause telangiectasia such as biological or congenital causes including:
- Klippel-Trenaunay syndrome
- Sturge-Weber syndrome
- Maffucci’s syndrome
- Ataxia-telangiectasia
- Osler-Weber-Rendu syndrome
- Naevus flammeus
There are also several acquired causes that can be brought on by a variety of other health and lifestyle factors. The most common of these is venous hypertension.
Simply put, venous hypertension refers to flow abnormalities and is often found alongside varicose and spider veins. Several factors can contribute to this including age, gender, pregnancy, and lifestyle.
Venous hypertension typically occurs between ages 18-35, peaking at around 50 or 60, although it can occur at any stage of life. Men are up to four times less likely to suffer from venous hypertension than woman. This is partially due to the effects of pregnancy on the walls of a woman’s blood vessels: As the hormones in her blood rise, they can damage and weaken these walls while an increase in blood volume causes distension in the veins. This can lead to pooling of the blood, venous hypertension, and telangiectasia.
Other causes
Many skin conditions or environmental factors may cause the appearance of telangiectasia. This includes:
- Acne rosacea
- Exposure to cold or direct sunlight
- Trauma to skin such as surgical incisions or injury
- Blepharitis
- Radiation exposure
- Chemotherapy
- Some forms of sclerosis or scleroderma
- Carcinoid syndrome
- Tempi syndrome
Some experts also warn that prolonged usage of topical corticosteroids may lead to the development of telangiectasia and spider veins.
Treating Telangiectasia
Typically, treating telangiectasia is performed with a process known as schlerotherapy, in which a medication is injected straight into the affected vein or capillary. This causes the vain to harden and shrink away, reducing the appearance of red and blue marks through the skin. Other treatments currently available include radiofrequency ablation, open surgery, and endovenous laser treatment.
Depending on what your clinic offers, you clients could have several options available to them. Knowing what exactly causes telangiectasia is the first step in successful treatment. Professionalism roots in knowing all causes and treatments of the medical issues you’ll deal with, so education in telangiectasia background is essential in providing a good consultation experience for your patients.
